Non-Alcoholic Fatty Liver Disease (NAFLD) has quietly become one of the most common liver disorders worldwide—yet most people living with it don’t even know they have it.
Unlike alcohol-related liver disease, NAFLD develops in people who drink little or no alcohol. It is closely linked to modern lifestyle patterns: poor diet, sedentary habits, obesity, insulin resistance, and metabolic syndrome. What makes NAFLD dangerous is not just how common it is, but how silent it remains until significant liver damage has already occurred.
In this blog, we’ll break down what NAFLD really is, why it’s rising rapidly (especially in India), how it progresses, how it’s diagnosed, and—most importantly—what can actually be done to reverse it.
What Is Non-Alcoholic Fatty Liver Disease?
NAFLD is a condition in which excess fat accumulates in liver cells (hepatocytes) in people who consume little to no alcohol. Normally, the liver contains small amounts of fat. When fat makes up more than 5–10% of liver weight, it becomes pathological.
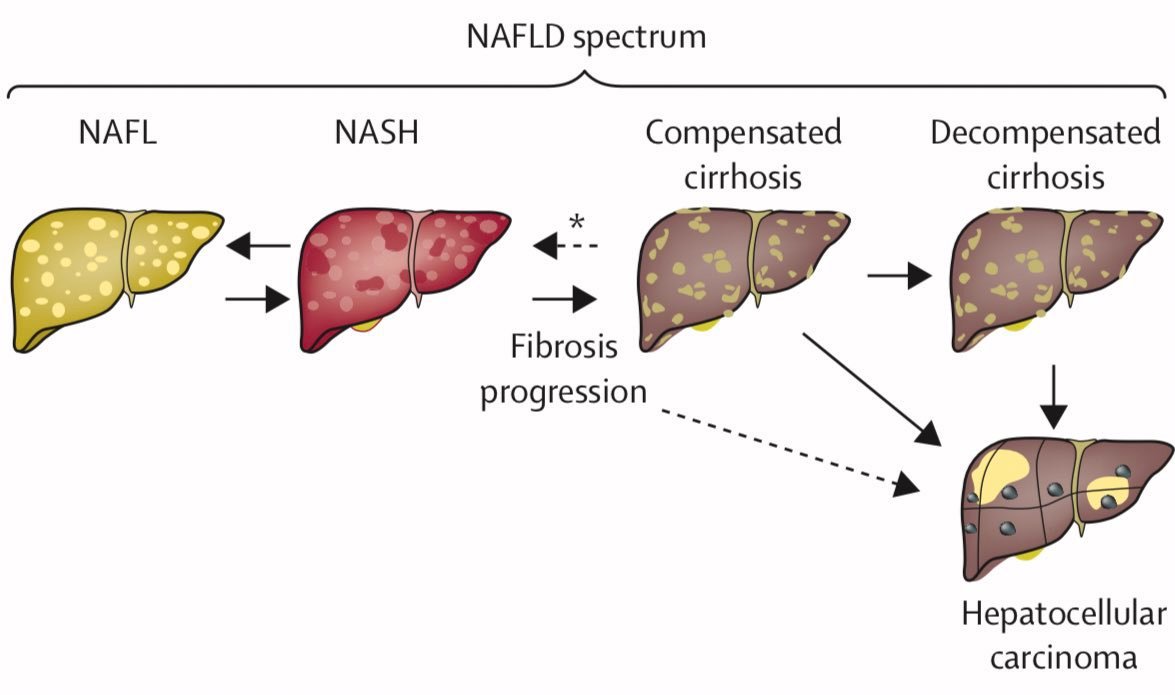
NAFLD is not a single disease—it is a spectrum:
- Simple fatty liver (steatosis)
- Non-alcoholic steatohepatitis (NASH) – fat + inflammation
- Fibrosis – scarring of liver tissue
- Cirrhosis – irreversible liver damage
- Hepatocellular carcinoma (HCC) in advanced cases
The frightening part? Many patients move along this spectrum without obvious symptoms.
Why Is NAFLD Increasing So Rapidly?
NAFLD is not really a “liver problem”—it’s a metabolic disease that shows up in the liver.
Major contributing factors include:
- Insulin resistance
- Central obesity (belly fat)
- Type 2 diabetes
- Dyslipidemia
- Sedentary lifestyle
- High intake of refined carbohydrates and sugar
- Ultra-processed foods
- In India, NAFLD is increasingly seen in:
- Young adults in their 20s and 30s
- People with normal BMI but high waist circumference
- Women with PCOS
- Patients with “borderline” blood sugar levels
This completely shatters the myth that only obese people develop fatty liver.
NAFLD vs Alcoholic Fatty Liver: A Common Confusion
One of the biggest misconceptions patients have is:
“Doctor, I don’t drink alcohol—how can I have fatty liver?”
NAFLD develops independently of alcohol. Even occasional social drinking does not protect against it. In fact, combining metabolic dysfunction with alcohol can accelerate liver damage.
So no—avoiding alcohol alone does NOT make you safe.
Symptoms: Why NAFLD Is Called a Silent Disease
Most people with NAFLD are asymptomatic.
When symptoms do appear, they are usually vague and easily ignored:
- Persistent fatigue
- Heaviness or discomfort in the right upper abdomen
- Bloating
- Poor digestion
- Brain fog
By the time clear symptoms like jaundice, ascites, or weight loss appear, the disease is often advanced
How Is NAFLD Diagnosed?
NAFLD is usually detected incidentally during routine investigations.
Common diagnostic tools include:
1. Blood Tests
- Mild elevation of ALT and AST
- Normal enzymes do NOT rule out NAFLD
- Liver enzymes can be normal even in fibrosis
2. Ultrasound Abdomen
- Increased liver echogenicity (“bright liver”)
- Cannot detect early fibrosis accurately
3. FibroScan (Transient Elastography)
- Measures liver stiffness and fat content
- Non-invasive and increasingly preferred
4. Liver Biopsy
- Gold standard
- Reserved for select cases due to invasiveness
⚠️ A critical mistake doctors and patients make is assuming that normal liver enzymes = healthy liver. That is simply false
NAFLD and Metabolic Syndrome: The Real Connection
NAFLD is strongly associated with metabolic syndrome:
- Abdominal obesity
- Hypertension
- High triglycerides
- Low HDL
- Elevated fasting glucose
Insulin resistance causes excess free fatty acids to flood the liver. Over time, this triggers oxidative stress, inflammation, and fibrosis.
In simple terms:
NAFLD is the liver’s way of saying your metabolism is broken.
Can NAFLD Be Reversed?
Yes—but only early and only with real lifestyle change, not cosmetic advice.
What actually works:
1. Weight Loss (Even 5–10%)
5% weight loss → reduces liver fat
7–10% → improves inflammation and fibrosis
Crash dieting is counterproductive. Slow, sustainable fat loss is key.
2. Dietary Changes (Not Fad Diets)
Effective dietary principles:
Reduce refined carbohydrates and sugar
Increase protein intake
Prefer whole foods over processed foods
Avoid sugary drinks and fruit juices
There is no single “fatty liver diet”—but metabolic control is non-negotiable.
3. Physical Activity
Resistance training + aerobic exercise works best
Exercise improves insulin sensitivity even without weight loss
Sedentary behavior is one of the strongest predictors of disease progression.
Role of Medications and Supplements
Currently, no drug is officially approved specifically for NAFLD.
Some medications may be used selectively:
- Insulin sensitizers
- Lipid-lowering agents
- Vitamin E (in specific cases only)
- Blindly taking “liver tonics” or herbal supplements without medical guidance can worsen liver injury
NAFLD and Cardiovascular Risk: The Bigger Threat
Most patients with NAFLD do not die from liver failure.
They die from heart attacks and strokes.
NAFLD is now recognized as an independent risk factor for cardiovascular disease. Ignoring fatty liver means ignoring the heart.
NAFLD in Lean Individuals: A Dangerous Myth
A growing number of patients with NAFLD are lean.
This condition—often called lean NAFLD—is common in South Asians due to:
- High visceral fat
- Genetic predisposition
- High carbohydrate diets
- So if you think:
- “I’m not overweight, so I’m fine”
- You may be very wrong.
When Should You Take NAFLD Seriously?
- You should NOT ignore fatty liver if:
- You have diabetes or prediabetes
- You have PCOS
- You have central obesity
- You feel chronically fatigued
- Your ultrasound repeatedly shows fatty liver
Early intervention can prevent irreversible liver damage.
Late intervention cannot.
Final Thoughts: NAFLD Is a Warning, Not a Diagnosis
Non-Alcoholic Fatty Liver Disease is not just a liver condition—it is a wake-up call.
It reflects deeper metabolic dysfunction that, if ignored, can progress to cirrhosis, liver cancer, and cardiovascular disease. The good news is that NAFLD is largely reversible in its early stages.
But reversal requires honesty, discipline, and consistency—not shortcuts.
Your liver doesn’t need magic pills.
It needs metabolic respect.